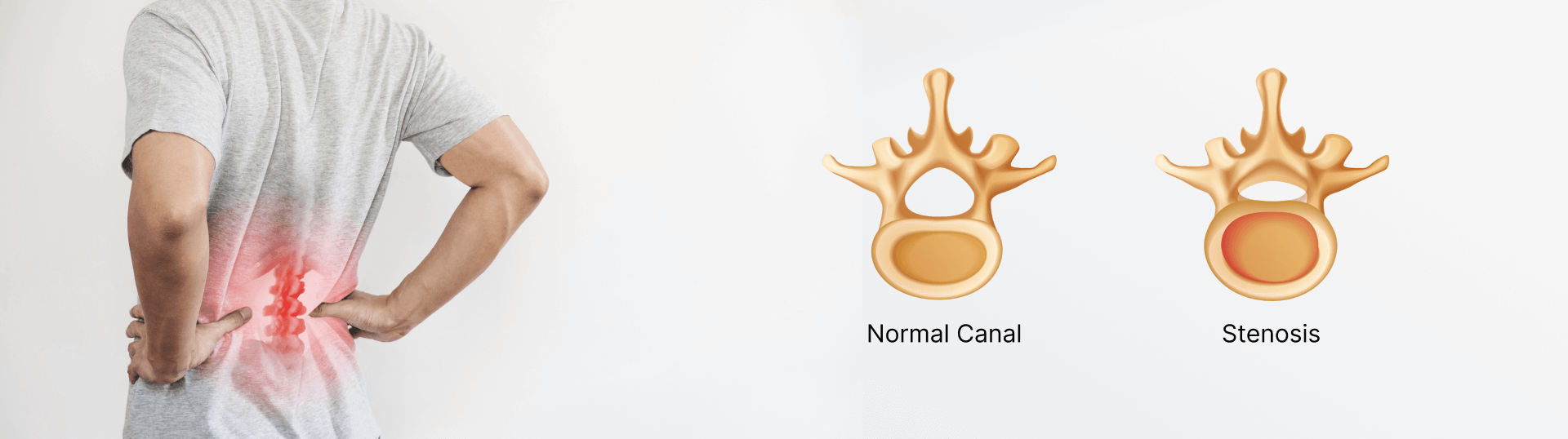
Spinal Stenosis
Spinal canal serves as the tunnel running through each vertebra in your spine, housing the spinal cord. Spinal stenosis occurs when the spinal canal narrows down. The lower back, legs, neck, shoulders, or arms may experience discomfort, cramping, weakness, or numbness as a result of this compression of the spinal cord and nerves. Spinal stenosis is a risk for people over 50 years of age. This ailment frequently results from changes brought on by aging, like osteoarthritis or bony spurs. Other potential causes include bulging discs or thickening of the ligaments. Higher risks are associated with females.
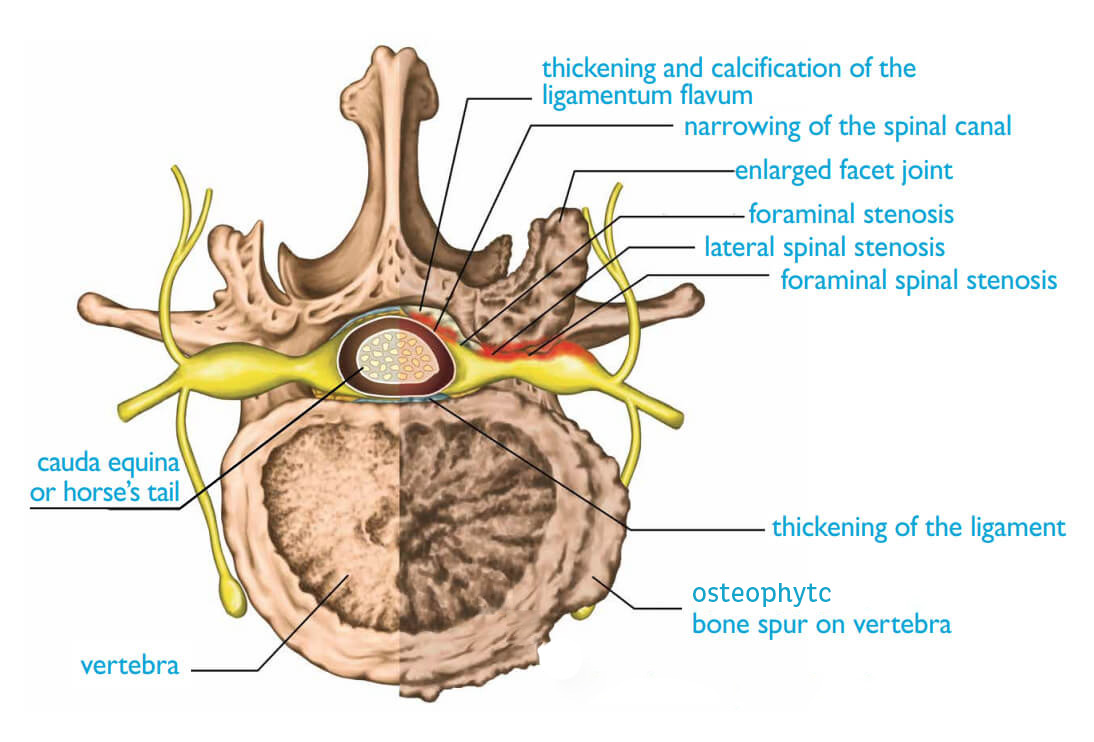
Stenosis most commonly affects two areas of your spine:
- Lower back: Called Lumbar canal stenosis
- Neck: Also called Cervical stenosis
Your middle back (also called the thoracic spine) can also have spinal stenosis, but this is rare.
Symptoms
Spinal stenosis occurs when the spaces within your spine narrow, putting pressure on the spinal cord and nerves. This compression can lead to a range of symptoms that affect your mobility and overall quality of life.
Common Stenosis Symptoms include:
Back Pain: Persistent pain in the lower back or neck. The pain may radiate down the arms or legs, depending on where the narrowing occurs.
Numbness and Tingling: Many individuals with stenosis experience numbness, tingling, or a "pins and needles" sensation in the arms, hands, legs, or feet.
Weakness: Muscle weakness, particularly in the arms or legs, can result from nerve compression caused by spinal stenosis.
Difficulty Walking: Hallmark of spinal stenosis - Stenosis can make walking and standing for extended periods challenging due to pain and discomfort. Some individuals may notice improvement when leaning forward or sitting.
Bowel or Bladder Dysfunction: In severe cases, spinal stenosis may affect bowel and bladder control, necessitating immediate medical attention.
What does spinal stenosis pain feel like?
The pain associated with spinal stenosis can vary significantly from one individual to another. For some, it may manifest as a persistent, dull ache or tenderness, while others may experience it as a sensation akin to electricity or burning. The pain can come and go.
Causes
Stenosis can be caused by a variety of factors. Many different changes or injuries in your spine can cause a narrowing of your spinal canal. The primary causes include:
- Aging: As we age, the spinal structures, including the discs and joints, can undergo degenerative changes that contribute to the narrowing of the spinal canal.
- Herniated Discs: Discs that bulge or herniation can put pressure on the spinal nerves and contribute to canal narrowing.
- Thickened Ligaments: Over time, the ligaments that support the spine can become thicker and contribute to the narrowing of the canal.
- Bone Spurs: Abnormal bone growth, known as bone spurs or osteophytes, can form within the spinal canal, reducing the available space for nerves.
- Congenital (from birth): Individuals may be born with a narrow spinal canal which makes them more susceptible to developing stenosis.
- Tumors: Tumors or abnormal growth within the spinal canal can compress the spinal cord or nerve roots, leading to stenosis.
Above mentioned are a few common causes of spinal stenosis, but each case can be unique.
Diagnosis
Diagnosing Spinal Stenosis
To diagnose spinal stenosis, your spine consultant will start by taking your medical history and conducting a physical exam to assess your pain and symptoms. Endospine360 Spinal stenosis doctors are specially trained to examine several different spinal conditions. You will be asked about your symptoms, including when they started, their severity, and any factors that exacerbate or alleviate them.
Your doctor will start diagnosis by clinical examination. Your doctor may also suggest imaging tests, such as X-ray, magnetic resonance imaging (MRI) scan, or computerized tomography (CT) scan.
At EndoSpine360 we follow patient-centric approach to diagnose Lumbar canal spinal stenosis and Cervical spinal stenosis. Endospine360 leverages state-of-the-art diagnostic tools and the expertise of highly skilled spine specialists.
Treatment
At EndoSpine360, we understand that each individual's experience with spinal stenosis is unique, and our treatment approach is also based on that.
If your symptoms are mild, our spine specialists may recommend at-home care first. If these methods don’t work, we take this further with physical therapy and medications as per the condition.
At-home care for spinal stenosis
This is suggested at the very initial stage when the patient has very mild symptoms. It may include:
- Applying heat which relaxes your muscles and relieves aching joints.
- Applying cold pack. It reduces swelling, tenderness, and inflammation.
- Exercises, which helps strengthen your core muscles to support your spine and improve flexibility and balance.
Non-surgical treatment for spinal stenosis
Non-surgical approaches are often recommended before considering surgical intervention. Non-surgical spinal treatment may include:
- Oral Medication: Over-the-counter pain relievers and muscle relaxants can help manage pain and inflammation.
- Epidural Steroid Injections: Corticosteroid injections can provide temporary relief by reducing inflammation and pain around the affected nerves.
Surgery for spinal stenosis
In some cases, your spine consultant might find the need for Surgery. It depends on the severity of your condition. At Endospine360 our goal of surgery is to relieve pressure on the spinal cord or nerve roots and restore spinal stability. Following are a few surgical options offered by Endospine360 spine specialists:
There are several surgical procedures used to treat spinal stenosis:
A. Decompression: It involves removing or trimming the structures that are compressing the spinal cord or nerve roots.
- OPEN (Laminectomy)
- Minimally Invasive
- Endoscopic
B. Decompression + Fusion Interbody: Spinal fusion surgery permanently joins (fuses) two vertebrae together using bone grafts or metal hardware or interbody cages. Spinal fusion stabilizes the spine and reduces motion in the affected vertebra.
- Open Fusion
- Minimally Invasive Interbody Fusion
- Endoscopic Surgery Interbody Fusion
Deciding on surgery necessitates careful consideration of the severity of your condition and consultation with your spine consultant. Our spine specialists at Endospine360 work together with patients to identify the necessity of surgery and with very careful consideration of the condition and personalized treatment plan is suggested.